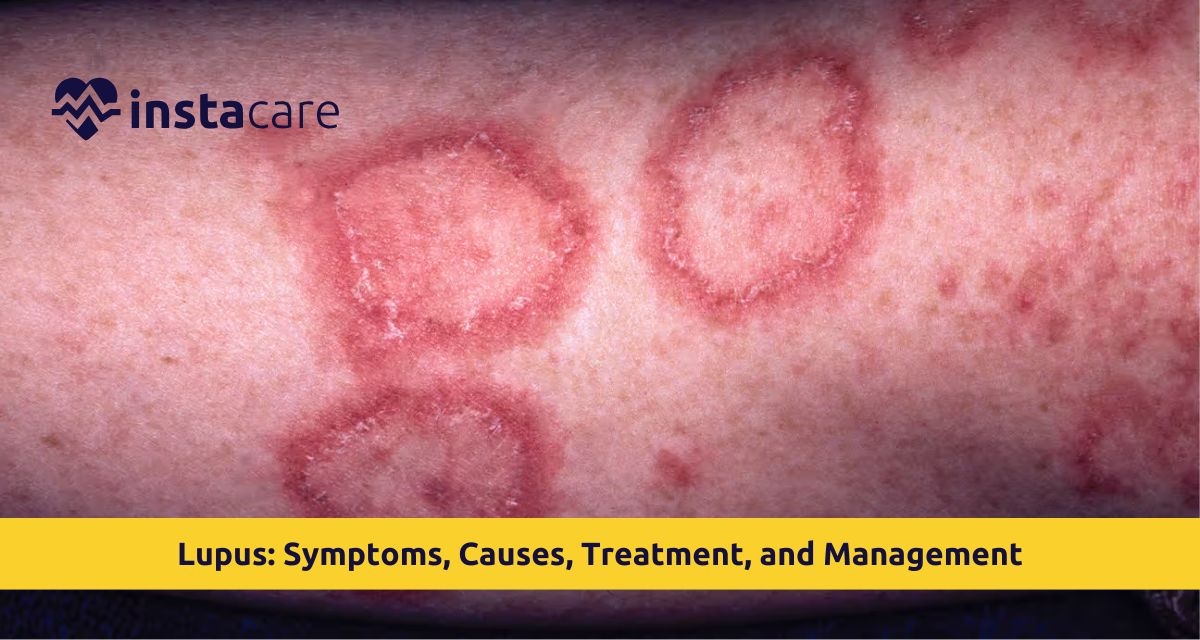
What is Lupus?
Lupus and autoimmune disease connection exists when the immune system of the body is hyperactive and targets the body's normal, healthy tissue with an autoimmune attack. Instead of being a protective shield against disease and infection, the immune system produces antibodies that kill the body's own cells, bringing pain,
inflammation, and organ damage.
Types of lupus come in different forms, the most common and dangerous one being systemic lupus erythematosus (SLE). SLE affects more than one organ system like skin, joints, kidney, heart, lungs, vessels, and brain. Discoid lupus (limited to the skin only), drug-induced lupus (secondary to some drugs), and neonatal lupus (an illness affecting new-born babies) are there.
The illness typically follows a flare-and-remission course. Lupus flare-ups consist of exacerbations of previous manifestations and onset of new manifestations, and remission is relief with disappearance of manifestations.
Causes and Risk Factors
The cause of lupus is still unknown but researchers attribute the disorder to the cause of the illness by virtue of the synergistic effect of environmental, genetic, and hormonal factors. Lupus causes are not inherited but genes with markers render an individual susceptible to the disorder.
Environmental triggers may induce lupus in a genetically predisposed person. The triggers for this are:
- Sunlight
- Viral and bacterial infections
- Stress
- Drugs
The hormonal factor cannot be overemphasized, therefore susceptibility of women of childbearing age to lupus.
Risk factors with greater probability of causing lupus are:
- Lupus in women - female gender since women's lupus is nine times more than lupus in men
- Age is a factor of role since the diagnoses also come most commonly in ages between 15 and 45 years
- Ethnicity is a factor of role with African American, Hispanic, Asian, and Native American being more susceptible and with more severe symptoms compared to Caucasians
- Genetic background is also a causative risk for increased susceptibility, yet most of those who have lupus have no one in their family who had this disease
Common Symptoms of Lupus
Lupus symptoms vary in each individual and is therefore not an easy disease to diagnose. Butterfly or lupus rash on cheeks and across the nasal bridge is seen in the majority of the patients. Facial flushing is also increased in sunlight.
In addition to the characteristic rash, features of classical lupus include:
- Profound fatigue that is unresponsive to rest
- Arthralgia in multiple joints and edema in multiple joints
- Spontaneous fever
- Photosensitivity in which sun exposure precipitates or aggravates the disease
- Alopecia or hair loss
- Mucous membrane lesions
- Raynaud's phenomenon, in which fingers and toes turn blue and white in cold temperatures
Lupus complications arise when the disease infects organs of the body's middle segment. Lupus and kidney disease (lupus nephritis) arises when infection of inflammation infects the kidney and leads to failure if not treated. Cardiovascular sequelae arise in the form of increased risk for heart lining or muscle and heart disease inflammation.
Cough and chest pain may be presenting symptoms as the lung is infected and inflamed. The neurologic presentation varies from headache and forgetfulness to seizures and psychosis in its most terrible form. Blood disorders are common in lupus and include anemia, clotting tendency, and coagulopathies. Side effects cost an expensive amount in quality of life and should be monitored carefully.
Diagnosis of Lupus
Lupus diagnosis is not easy because all the other diseases imitate it and there is no absolute test for diagnosis. Physicians relied on a mix of history, physical examination, and a few laboratory tests. The American College of Rheumatology defined criteria for eleven features such as:
- The characteristic butterfly rash
- Photosensitivity
- Oral ulcers
- Arthritis
- Renal disease
- Neurologic impairment
- Blood dyscrasias
- Immunologic laboratory tests
- A positive antinuclear antibodies (ANA)
Four or more are the norm but physicians diagnose on fewer.
The diagnosis of lupus requires blood tests to be conducted. ANA testing is also used for screening for autoantibody, but a positive result will not establish the diagnosis of lupus since other illnesses will be positive ANA as well. Complete blood count, kidney and liver function tests, urine test, and specific antibody testing are helpful in diagnosis-making and disease activity assessment.
Treatment and Management
While lupus cannot be cured, lupus treatment is focused on managing the symptoms, averting the flare-ups, and protecting against organ damage. The treatment is highly personalized to the extent of symptoms and which organs are involved.
Medications are the cornerstone of lupus therapy:
- NSAIDs alleviate pain and inflammation
- Antimalarial drugs like hydroxychloroquine control lupus disease and flares
- Corticosteroids eliminate inflammation quickly but should be used cautiously due to side effects if required long-term
- Immunosuppressants quiet an overactive immune system, usually in serious lupus or if the organs become involved
- Biologics are more recently developed medications that inhibit specific components of the immune system
Treatment is backed by adaptation to life. Sun avoidance is very important as ultraviolet light triggers flares. Use of high-SPF sunscreen, protective clothing, and sun cover at peak sun times is advised. Maintenance of regular exercise such that reduced mobility of the joints, muscle power, and cardiovascular function without triggering chronic fatigue.
Stress-reducing exercises, meditation, or counseling reduce stress, thereby causing prevention of stress flares. Rest and uninterrupted sleep for flares so that the body can heal. Fruit and vegetable diet supplemented with
omega-3 fatty acids is otherwise normal and helps to eradicate inflammation.
Living with Lupus
Lupus as an uncertain and chronic disease necessitates living with lupus adjustments. Patients live active, normal lives through collaborative collaboration with doctors and modification of lifestyle habits.
One needs a support network. Support networks consisting of other lupus victims provide emotional support as well as "hands-on" familiarity. Family members and friends who are educated about the disease are excellent sources of support in a crisis situation. Mental support for mental health in therapy or counseling environments allow for coping with the emotional pain of chronic disease.
For survival with lupus, much improved is the prognosis with the new management. Lupus life expectancy in the majority of cases of lupus is almost as good as in nonlupus patients, if one is diagnosed early and treated in the right way. Prognosis depends upon severity of disease, organs affected, and response to therapy. Follow-up drug and clinical is the key to long-term success.
Care has to be exercised particularly in lupus women during planning for pregnancy. Pregnancy can be made safe in the majority of women, but not a lupus-safe pregnancy. Multidisciplinary care by high-risk experienced obstetricians and rheumatologists is the best means of obtaining the best outcome.
Conclusion
Lupus is still a mysterious autoimmune disease that attacks patients at random, yet identification of the signs of lupus, prodromal warning symptoms, and prompt evaluation significantly enhances the outlook. As difficult as it is to be a lupus patient, the quality of treatment and management makes it feasible for the majority of patients to live healthy, productive lives.
By proper management of the disease with medicine, modification in lifestyle, and supportive social interaction, patients with lupus can manage the disease and reduce its impact on activities of daily living. Research is ongoing to explore new avenues to the disease and promise better therapy and eventually a cure.
Please book an appointment with the
best Dermatologist in Lahore, Karachi, Islamabad, and all major cities of Pakistan through
InstaCare, or call our helpline at 03171777509 to find the verified doctor for your disease.